Why Your Practice is Losing Money to Rejected and Denied Claims (And How AI Can Help)
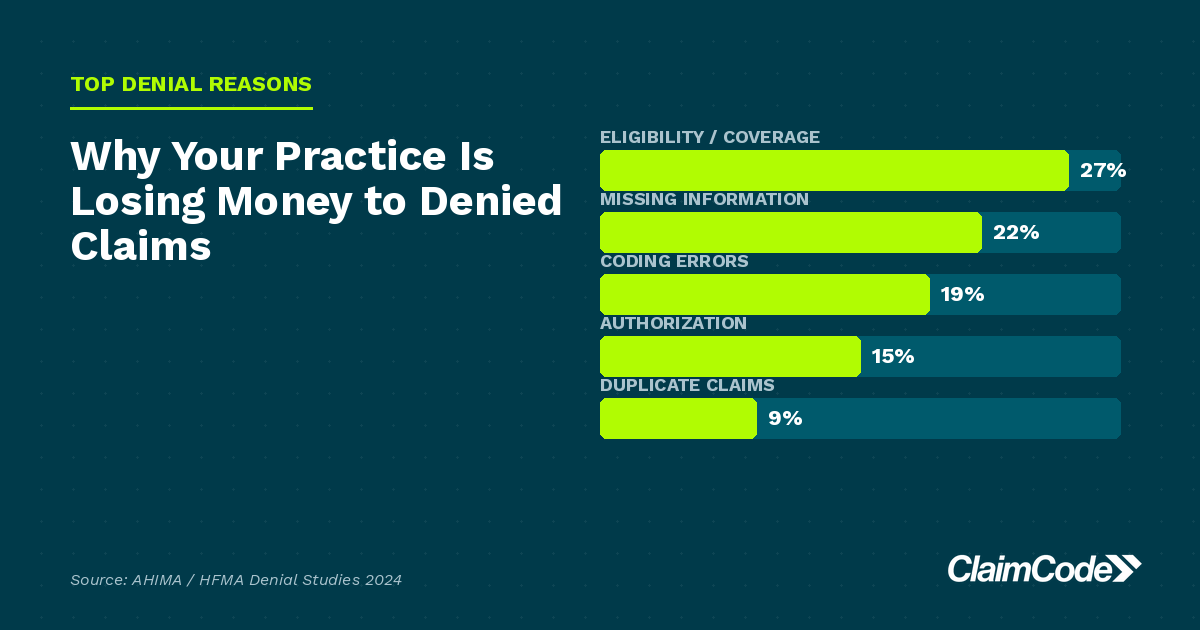
Understand why insurance companies deny your claims and how AI-powered revenue cycle intelligence helps wellness practices recover lost revenue faster.
Every week, your practice submits claims to insurance companies. Some get paid. Some don't. Do you know why?
If you're like most wellness practitioners, the answer is probably "not really." You know certain claims got rejected or denied, but understanding exactly what went wrong — and how to fix it — feels like decoding a foreign language.
About 20% of medical claims are denied, rejected, or underpaid. Up to 60% of those are never resubmitted. That revenue disappears from the practice.
For a 5-provider physical therapy practice billing $750,000 annually, that's $90,000 to $150,000 a year lost to claims that were never properly managed.
This is a solvable problem. Automated claim tracking and plain-English denial explanations close most of the gap.
The Hidden Complexity of Insurance Claims
When you submit a claim to an insurance company, it passes through multiple review stages before you (hopefully) get paid. Understanding those stages is how you protect your practice's revenue.
Stage 1: Initial Validation
Before an insurance company even looks at your claim, it runs through automated validation checks. These systems verify that:
- All required fields are filled out correctly
- Provider and patient information matches their records
- The claim is properly formatted
- You're not submitting a duplicate
If your claim fails any of these checks, it gets rejected immediately. The insurance company's system essentially says, "We can't process this—fix it and send it back."
Common rejection reasons include:
- A typo in the patient's insurance ID number
- Missing or incorrect provider NPI
- Wrong date format
- Mismatched patient name
The key thing to understand about rejections: your claim never actually entered the insurance company's payment system. It was stopped at the door. This means you can fix the error and resubmit—but it also means your timely filing clock is still ticking.
Stage 2: Adjudication (The Review Process)
If your claim passes validation, it moves to adjudication. This is where the insurance company actually reviews the services you provided and decides what—if anything—they'll pay.
During adjudication, they check:
- Is the patient's coverage active for these dates?
- Are these services covered under the patient's plan?
- Do the diagnosis codes support the treatment codes?
- Are there any coordination of benefits issues (multiple insurance plans)?
- Does this claim require prior authorization?
If something goes wrong here, your claim gets denied. Unlike a rejection, a denial means the insurance company received your claim, reviewed it, and decided not to pay it (or to pay less than you billed).
Denial reasons are often more complex:
- Service not covered under the patient's plan
- Missing prior authorization
- Treatment exceeded visit limits
- Diagnosis doesn't support the procedure
- Coordination of benefits issues
Here's the critical difference: once a claim is denied, you typically can't just fix it and resubmit. Many payers require a formal appeals process, which takes time, effort, and expertise.
Why This Matters for Wellness Practices
Physical therapy, occupational therapy, and chiropractic practices face unique billing challenges that make claim management even more critical.
The 8-Minute Rule
PT and OT practices must carefully track time-based therapy codes. Bill incorrectly, and your claim gets denied—even though you provided the service.
Multiple Procedure Payment Reduction (MPPR)
When you provide multiple therapy services in the same session, insurance companies often reduce payment for subsequent procedures. If you don't account for this correctly, you'll be caught off guard by underpayments.
Maintenance Care Limitations
Chiropractic practices frequently deal with denials around maintenance care versus active treatment. Documentation requirements are strict, and phrasing matters enormously.
Medicare Part B Therapy Caps
Even though therapy caps have exceptions, tracking them and submitting the necessary documentation is complex. Miss a step, and you're facing a denial.
The specialized nature of wellness practice billing means generic billing software often misses these nuances. You need tools that understand your specialty's specific requirements.
The Real Cost of Ignored Claims
Let's talk numbers. According to the American Academy of Family Physicians, the industry average denial rate sits between 5% and 10%. But here's the shocking part: only 35% of providers appeal denied claims.
Why? Because working denied claims is:
- Time-consuming: Staff spend hours researching denial reasons, gathering documentation, and writing appeal letters
- Complex: Understanding insurance policies and appeal procedures requires specialized knowledge
- Demoralizing: After weeks of work, many appeals are denied anyway
So practices make a business decision: it's not worth the effort. They write off the revenue and move on.
But when you add up all those written-off claims—plus the rejections that never got fixed, plus the underpayments nobody noticed—you're looking at a significant revenue leak.
What ClaimCode Does
ClaimCode works alongside your existing billing setup as a complementary analytics layer. Instead of your staff manually tracking down claim responses, decoding cryptic insurance codes, and figuring out next steps, ClaimCode runs that work in the background — built specifically for wellness practices.
Automatic Claim Monitoring
After you submit a claim (through your existing system), ClaimCode automatically:
- Monitors for responses from insurance companies
- Captures both immediate rejections and later denials
- Tracks partial payments and underpayments
- Organizes everything by claim status and reason
No more logging into multiple clearinghouse portals. No more waiting for paper remittances. Everything you need is in one place.
Plain-English Denial Explanations
Insurance companies send back coded responses that look like this:
Status Code: A7:562:1P
Without ClaimCode, a billing manager looks up multiple codes and figures out which provider and which NPI field caused the issue. ClaimCode decodes the response and returns a plain-English explanation your team can act on.
Patterns Across Your Practice
ClaimCode doesn't just explain individual claims—it helps you see patterns across your entire practice:
- Denial Trends: Which insurance companies deny your claims most often? Which procedure codes are problem areas?
- Provider-Specific Issues: Is one practitioner having more claim problems than others?
- Financial Impact: How much revenue is sitting in rejected or denied claims right now?
- Time-to-Payment Metrics: How long does each payer take to process claims?
The Bottom Line: Protect Your Revenue
Every rejected claim is one you can fix and resubmit. Every denial is a decision point: is this worth appealing, or should we prevent this issue next time? You can't manage what you can't see, and you can't fix problems you don't understand.
ClaimCode shows you every claim's status in one place, translates the payer's response into plain English, and gives your team clear next steps. Over time, the pattern view surfaces which payers, procedure codes, and providers account for most of the denial pressure — so you can stop them upstream instead of chasing them after the fact.
For a typical wellness practice, that 10-20% of revenue slipping past the billing team adds up to $100,000-$200,000 a year. Recovering most of it doesn't require more headcount. It requires visibility into what the payer is actually telling you.
Related Reading
Denied Outpatient Claims Rose 14% in 2025. Here's What That Costs the Average PT or Chiro Practice.
Denied outpatient claim amounts rose 14% in 2025. Here's what the math means for PT and chiro practices — and how to stop the revenue from walking out the door.
What the UHC Prior Auth Expansion Means for Your PT and Chiropractic Billing Team
UHC's Medicare Advantage prior authorization program keeps expanding. Here's what the 6-visit waiver actually covers — and where the documentation traps are.

Dr. Andrew O'DonnellPhD, LSSGB
CEO and founder of ClaimCode. Expert in insurance analytics, digital transformation, and business operations. Passionate about helping private wellness practices manage their revenue cycle with meaningful insights.
Ready to stop losing revenue to denied claims?
ClaimCode gives your billing team real-time claim visibility and AI-powered remediation guidance — at flat-fee pricing.
Get Early Access