Revenue Cycle Intelligence Built for Wellness Practices
Empower your billing team with AI-powered insights, specialty-specific guidance, and industry benchmarking—built specifically for wellness practices.
AI-Powered Claim Analysis
Understand Every Denial in Seconds, Not Hours
- Decode payer response codes automatically
- Get specialty-specific explanations
- Receive step-by-step remediation instructions
- Track appeals and resubmissions
Use Case: When Blue Cross denies your claim with 'CO-16: Claim lacks information,' ClaimCode tells you exactly which documentation is missing and how to get it.
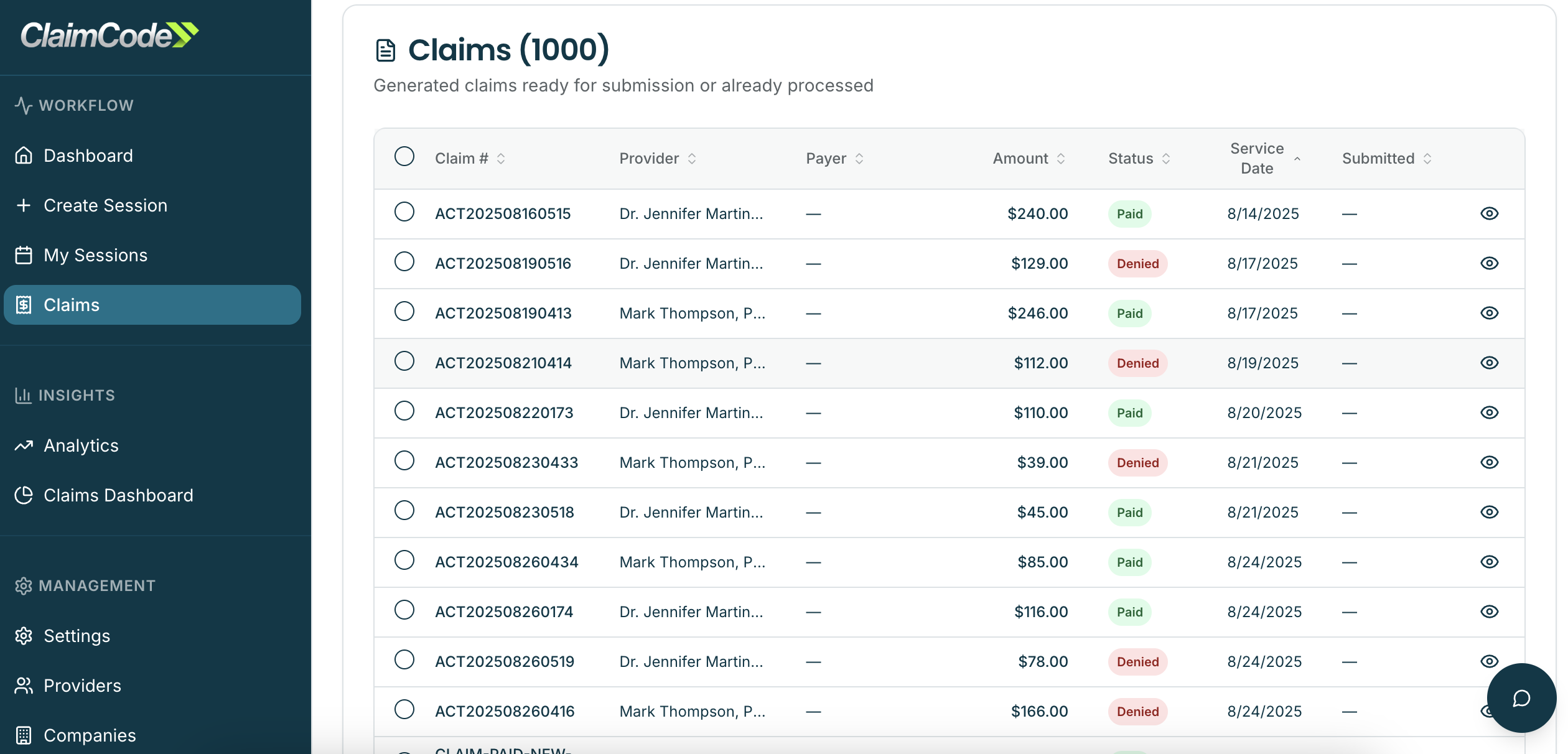
Comprehensive Claim Monitoring
100% Visibility Across Your Entire Revenue Cycle
- Monitor revenue throughout the claims lifecycle
- Real-time alerts for rejections and denials
- Track partial payments and underpayments
- Identify abandoned claims before they're forgotten
47.5%
47.5% - The percentage of denied claims that are abandoned by a typical wellness practice.
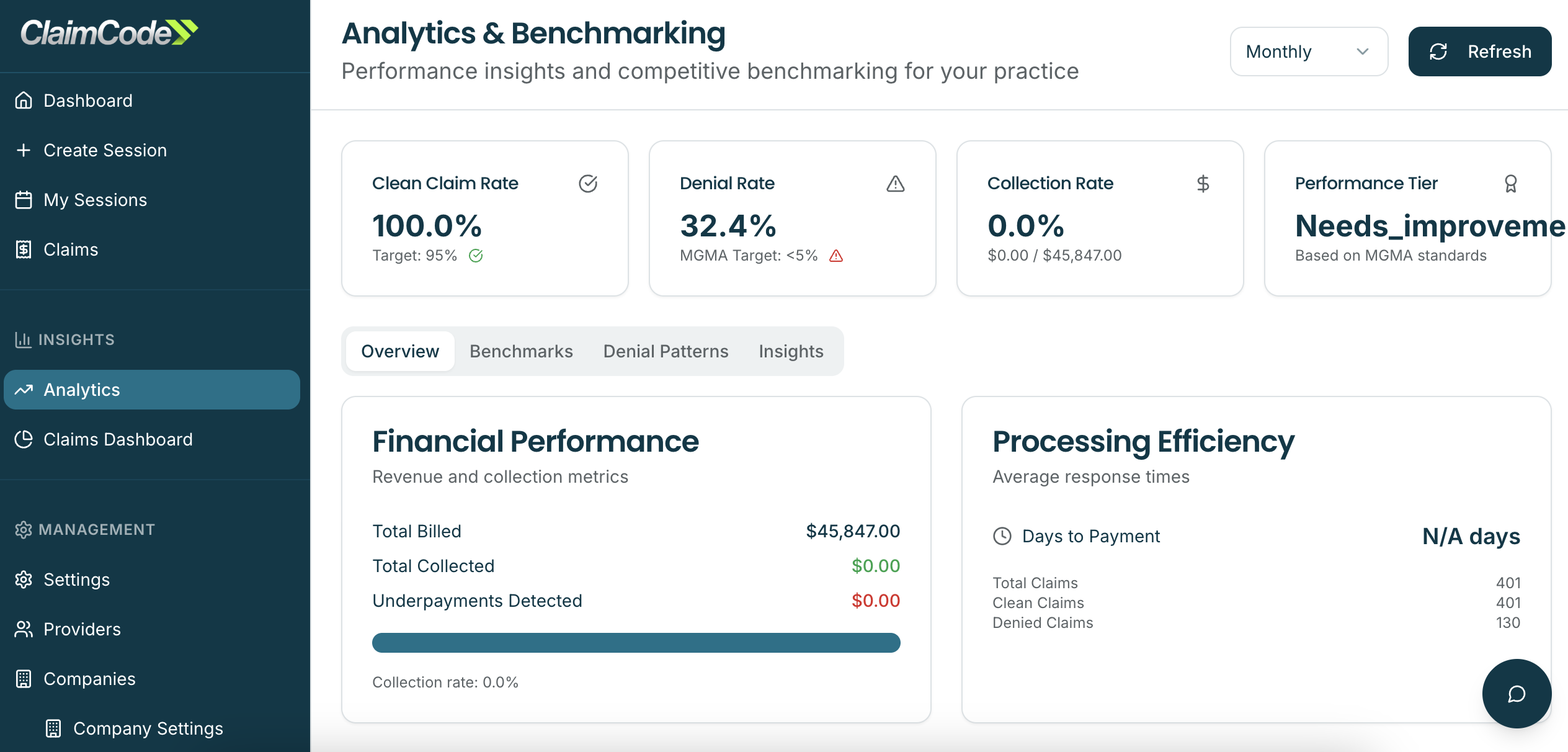
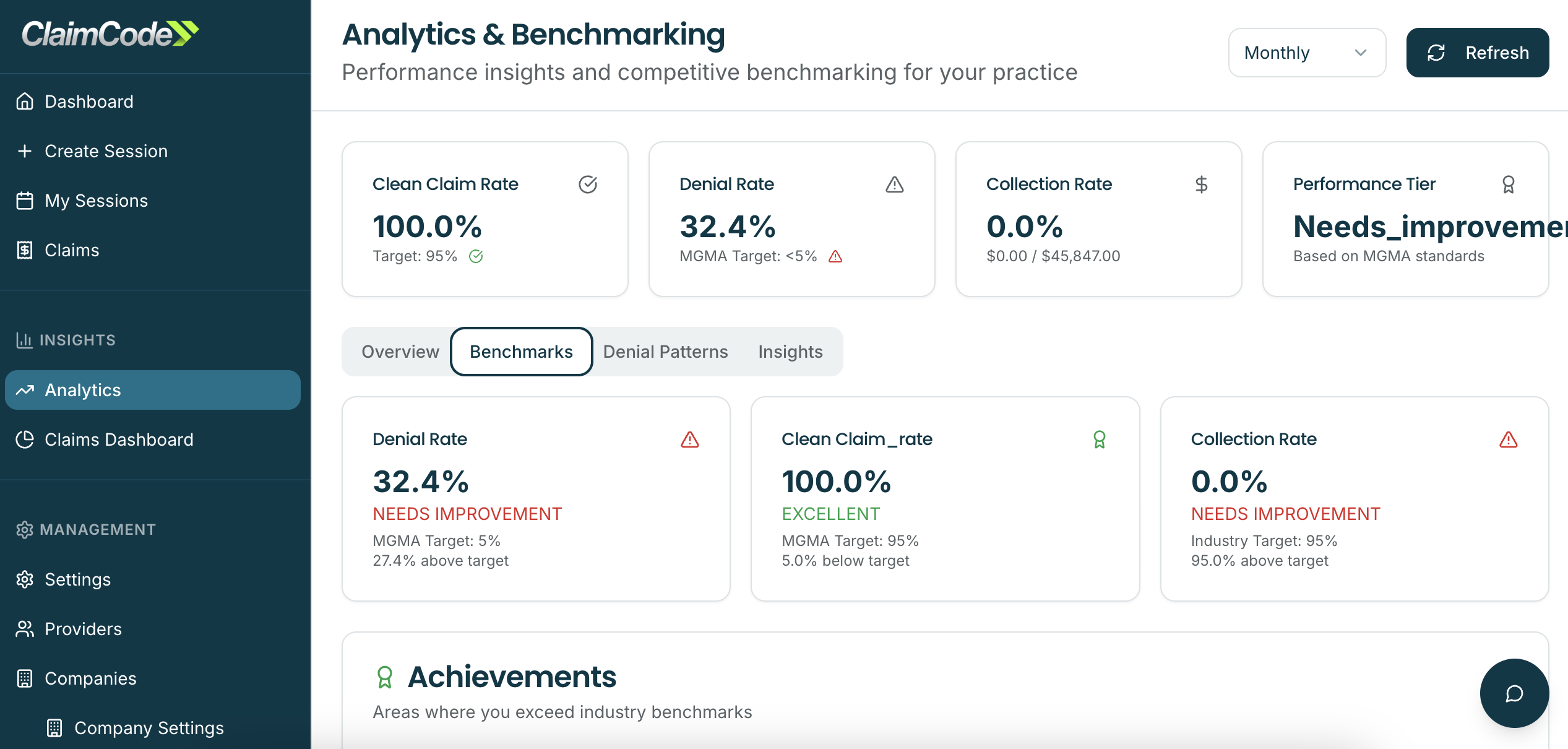
Industry Analysis & Insights
Know Where You Stand
- Compare denial rates against similar practices
- Identify problematic payers regionally
- Track performance trends over time
- Validate RCM team effectiveness
Only platform providing comprehensive wellness practice industry analysis data
Works Alongside Your Existing Workflow
Complements your existing workflow without replacing the tools you already use.
Connect to 500+ payers for real-time claim status checks
No system replacement
Rapid setup
Real-time tracking